Infectious Mononucleosis (传染性单核细胞增多症): Complete Chinese Dietary Therapy Protocols
Infectious mononucleosis, triggered by the Epstein-Barr virus (EBV), represents a major therapeutic challenge in Traditional Chinese Medicine (TCM). This acute viral pathology frequently evolves toward post-viral chronic fatigue patterns that deplete the body’s Qi and Yin. The dietary approach cannot simply be a static list of foods: it must be dynamic, differential and evolving, adapting to each clinical phase and the patient’s individual energy patterns.

When Wind and Heat invade the body, the Yang Qi becomes depleted; the Spleen loses its motive force and the Yin is consumed. Nourishing Qi and protecting Yin are the foundations of convalescence.
Differential Diagnosis in TCM: Bian Zheng Lun Zhi (辨证论治)
The TCM approach requires rigorous differential diagnosis before any dietary prescription. Infectious mononucleosis traverses several energy patterns during its evolution, from external invasion of Toxic Heat to deep depletion of Qi and Yin. The Ba Gang (Eight Principles) matrix allows this analysis to be structured into three distinct clinical phases.
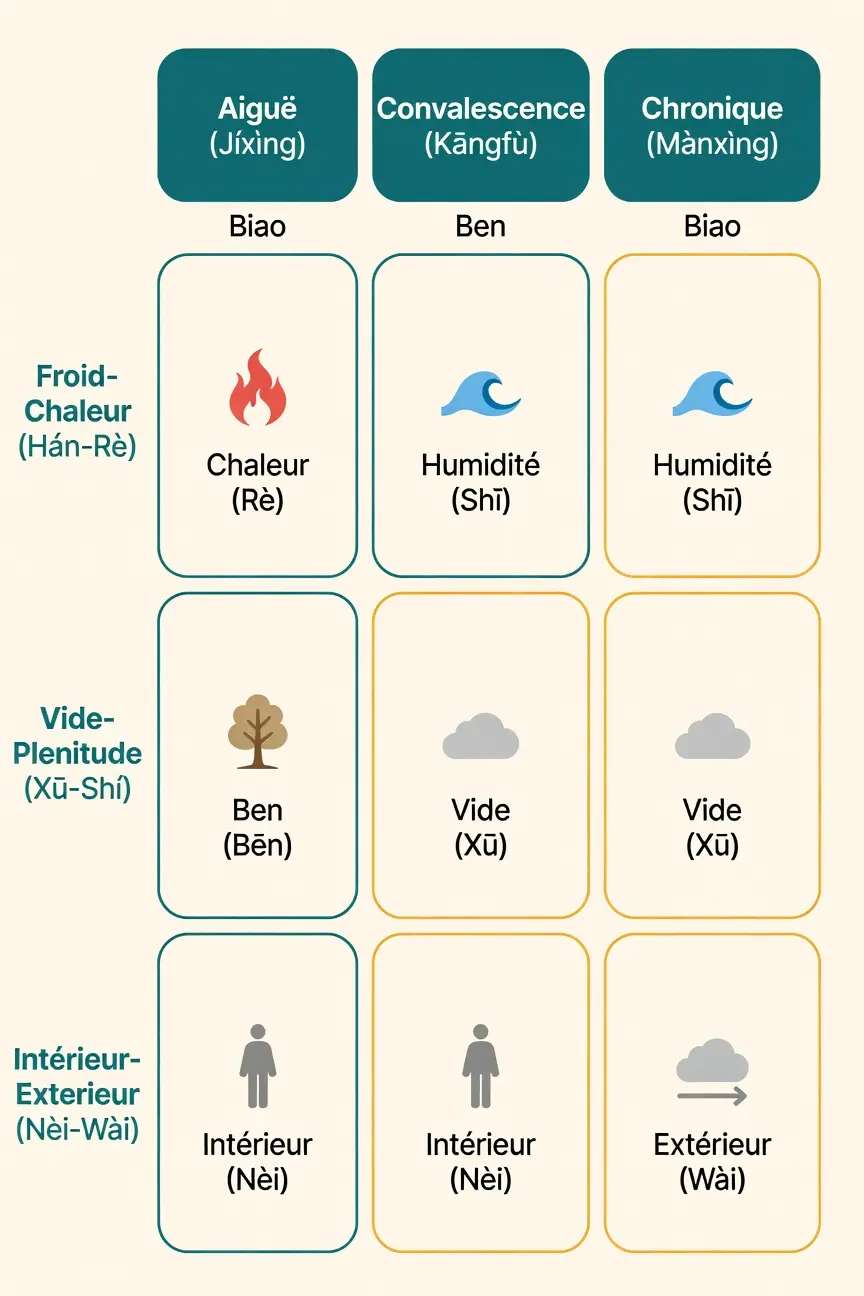
Analysis According to the Eight Principles (Ba Gang)
| Aliment | Nature | Saveur | Méridiens | Actions | Précautions |
|---|---|---|---|---|---|
| Biao/Ben | Acute Phase: Biao dominant (Toxic Heat) | Convalescence Phase: Biao/Ben transition | Chronic Phase: Ben dominant (Qi/Yin Deficiency) | Biao = surface, Ben = root; the illness progressively migrates in depth | Never tonify in pure acute Biao phase |
| Cold/Heat | Acute Phase: Excessive Heat | Convalescence Phase: Residual Heat + Deficiency | Chronic Phase: Cold Deficiency or Empty Heat | The thermal nature evolves with depletion of organic fluids | Distinguish Full Heat from Empty Heat before any treatment |
| Deficiency/Excess | Acute Phase: Excess of Toxic Heat | Convalescence Phase: Mixed - residual Excess + Deficiency | Chronic Phase: Qi, Blood, Yin Deficiency | Progressive transition from external excess to deep internal deficiency | Do not disperse in chronic phase; do not tonify in acute phase |
| Interior/Exterior | Acute Phase: External invasion in transformation | Convalescence Phase: Pathogen penetrating in depth | Chronic Phase: Latent pathogen, internal deficiency | The EBV virus passes from the Wei Qi layer to the Middle Jiao then the Lower Jiao | Monitor symptom migration: throat - spleen - kidney |
Differential diagnosis according to eight criteria - Yin Shi synthesis adapted to EBV
Pattern 1: Toxic Heat of Lung and Stomach (Acute Phase)
Clinical signs:
- High fever, bright red throat, exudative tonsils
- Intense thirst, preference for cold drinks
- Tongue: red, thick yellow coating; Pulse: rapid, slippery
Mechanism: Invasion of Feng-Re (Wind-Heat) transforming into Re-Du (Toxic Heat) that stagnates in the Upper Jiao. The EBV virus first attacks the upper respiratory tract, corresponding to the domain of Lung and Stomach in TCM.
Pattern 2: Damp-Heat Blocking the Middle Burner
Clinical signs:
- Heavy fatigue, sensation of heaviness, nausea
- Swollen lymph nodes, tender spleen
- Tongue: yellow-greasy coating; Pulse: slippery, soggy
Mechanism: Internal Dampness (weak Spleen) combines with external Heat, creating stagnation that obstructs Qi circulation in the Middle Jiao. Swollen lymph nodes translate accumulation of Phlegm-Dampness in the Spleen and Stomach meridians.
Pattern 3: Liver Qi Stagnation with Latent Heat
Clinical signs:
- Irritability, hypochondriac distension
- Fluctuating fatigue, sleep disturbances
- Tongue: red edges, pale body; Pulse: wiry
Mechanism: Prolonged illness affects the Liver, generator of free Qi circulation. Liver stagnation prevents complete resolution of Toxic Heat, which persists as latent heat. This pattern is frequent in adolescent and young adult patients, the population classically affected by mononucleosis.
Pattern 4: Lung and Spleen Qi Deficiency (Post-viral)
Clinical signs:
- Deep fatigue, breathlessness on exertion, spontaneous sweating
- Poor appetite, loose stools
- Tongue: pale, tooth-marked; Pulse: weak, deficient
Mechanism: The infection has depleted the defensive Qi (Wei Qi) and Spleen Qi, source of Qi and Blood production. The Lung, Master of Qi, and the Spleen, source of transformation-transportation, are the two organs most weakened by the acute febrile phase.
Pattern 5: Liver and Kidney Yin Deficiency with Empty Heat
Clinical signs:
- Fatigue with night restlessness, night sweats, dryness
- Dry mouth in the evening, mild irritability
- Tongue: red without coating, fissured; Pulse: thin, rapid
Mechanism: Prolonged Heat has consumed the organic fluids (Jin-Ye) and Yin, creating Empty Heat that sustains fatigue despite resolution of the acute infection. This pattern predominates in chronic forms and persistent post-EBV fatigue beyond 3 months.
Dietary Strategies by Pattern and Phase
Dietary prescription in TCM is not limited to a generic list of foods against mononucleosis. Each clinical phase imposes its own therapeutic principles, pivot foods and absolute contraindications. The therapist must adjust the strategy at each consultation, based on pulse evolution, tongue and functional symptomatology.
Phase 1: Acute (Day 1-14) - Clear Toxic Heat
In the acute phase, the fundamental principle is Qing Re Jie Du (Clear Heat and Resolve Toxins): clear the Heat and eliminate Toxins. Food must be liquid, slightly warm, and never burden digestion.

| Aliment | Nature | Saveur | Méridiens | Actions | Précautions |
|---|---|---|---|---|---|
| Toxic Heat Lung/Stomach | Qing Re Jie Du | Clear Heat, eliminate Toxins | Fresh, bitter, sweet; Lung, Stomach, Liver | Pear (raw or cooked), watermelon, melon, cucumber, celery, mung beans (Lu Dou), chrysanthemum, fresh mint | Fresh juices, light soups, warm infusions (never iced) |
| Damp-Heat | Qing Re Hua Shi | Clear Heat, resolve Dampness | Fresh, bitter, aromatic; Spleen, Stomach, Lung | Pearl barley (Yi Yi Ren), white radish (Daikon), zucchini, aubergine, light green tea, lemon (zest) | Barley congee, steamed vegetables, skimmed broths |
| Absolute Contraindications | To be avoided throughout the acute phase | Hot/spicy foods (chili, dried ginger, cinnamon), fried foods, animal fats, dairy products, refined sugar, alcohol | These foods nourish Heat and generate Phlegm-Dampness |
Clear Toxic Heat and resolve Dampness - Yin Shi prescriptions
Phase 2: Convalescence (Day 15-45) - Tonify without nourishing stagnation
Convalescence is a critical and unstable phase. The external pathogen is partly resolved, but Spleen and Lung Qi are already exhausted. Any brutal or premature tonification risks nourishing residual stagnation or a Heat rebound. Progression must be gradual and cautiously observed.
| Aliment | Nature | Saveur | Méridiens | Actions | Précautions |
|---|---|---|---|---|---|
| Spleen/Lung Qi Deficiency | Bu Qi Jian Pi | Tonify Qi, strengthen Spleen | Neutral to warm, sweet; Spleen, Lung, Kidney | Brown rice, millet, quinoa, sweet potato, pumpkin, farm chicken (broth), chestnut, cashew nuts, shiitake, oyster mushrooms | Nutritive congee, slow-cooked dishes, gentle steam cooking |
| Liver Qi Stagnation | Shu Gan Li Qi | Release Liver, circulate Qi | Fresh to neutral, sour, aromatic; Liver, Gallbladder | Spinach, rocket, watercress, lemon (juice), rice vinegar, basil, fresh coriander, steamed white fish | Quickly stir-fried green vegetables, light seasonings |
| Residual Heat | Qing Xu Re | Clear Empty Heat | Neutral to fresh, sweet, sour; Liver, Kidney | Goji berries (moderate), blackberries, blueberries, spinach, asparagus, black sesame (small quantities) | Light preparations, avoid long cooking that generates Heat |
Progressive Qi tonification and Liver release - Yin Shi prescriptions
Phase 3: Chronic / Post-viral Fatigue (Day 45+) - Reconstruct the Root
Beyond 45 days, persistent fatigue signals deep exhaustion of the Ben (energy root). Dietary treatment then aims to reconstruct Qi, Blood, Yin or Yang according to the dominant pattern. Regularity and consistency take precedence over quantity.

| Aliment | Nature | Saveur | Méridiens | Actions | Précautions |
|---|---|---|---|---|---|
| Liver/Kidney Yin Deficiency | Zi Yin Yang Xue | Nourish Yin, enrich Blood | Neutral to fresh, sweet, salty; Liver, Kidney, Heart | Quail egg, organic egg yolk, squid, cuttlefish, blackberry, goji berries, black sesame, walnut, spinach, beetroot | Nourishing soups, sweet slow-cooked dishes, avoid overcooking |
| Spleen/Kidney Yang Deficiency | Wen Bu Pi Shen | Warm and tonify | Warm to hot, sweet, salty; Spleen, Kidney, Heart | Lamb (moderate), farm chicken, cinnamon (small dose), fresh ginger, walnut, chestnut, red date, glutinous rice, oats | Sweet stews, warming spices added at end of cooking |
| Immune Support | Fu Zheng Gu Ben | Strengthen Zheng, consolidate the root | Variable; Lung, Spleen, Kidney | Astragalus (Huang Qi) in broth, medicinal mushrooms (Reishi, Shiitake), moderate raw garlic, spring onion, fresh ginger, turmeric | Long broths (4-6 hours) to extract active principles, accompanying infusions |
Root reconstruction: Qi, Blood, Yin and Yang - Yin Shi prescriptions
Specific Protocols by Dominant Symptom
Beyond general phases, certain persistent symptoms require targeted adjustments to the dietary prescription. The TCM therapist must identify the dominant pattern and adapt the protocol accordingly.
Persistent Post-viral Fatigue
TCM Pattern: Lung and Spleen Qi Deficiency, often associated with residual Dampness stagnation.
Dietary Approach: Combine Qi tonification and gentle drainage of residual Dampness.
Typical Food Protocol:
- Base tonifying congee: millet (30g), brown rice (20g), dried shiitake (5g), astragalus (Huang Qi, 3g in sachet) - slow cooking 90 minutes, taken warm first thing in the morning on an empty stomach
- Balanced lunch: steamed root vegetables (carrot, beetroot), organic white fish or poultry (60g), quinoa (40g, al dente cooking)
- Snack: goji berries (10g) infused in warm water, never on an empty stomach if the stomach is empty
- Light dinner: vegetable soup with kombu seaweed (3cm), no animal protein after 7pm
Persistent Swollen Lymph Nodes
TCM Pattern: Qi and Blood stagnation with Phlegm accumulation (Tan) in the Spleen and Stomach meridians.
Dietary Strategy:
- Draining foods: black radish (grated raw, 20g), kombu and wakame seaweed (infusion or soup), celeriac (steamed or grated raw)
- Avoid: dairy products, sugar, fried foods (all Phlegm-Dampness generators)
- Optimal preparation: root vegetables in fine julienne, raw or slightly blanched to preserve energetic dispersion action
Brain Fog and Concentration Difficulties
TCM Pattern: Heart and Liver Blood Deficiency, or Dampness obstructing the Heart orifices.
Dietary Strategy:
- Nourish Blood: cooked red beetroot, spinach (stir-fried or blanched), organic chicken liver (once a week, 80g maximum), goji berries (infusion morning and noon)
- Clarify the Spirit: infusions of lime flower (European matricary chamomile), white chrysanthemum, dried lotus flower
- Avoid: excess coffee and black tea (disperse the Shen), too large lunches (saturate the Middle Jiao and divert Blood from the head)
Contraindications and Specific Precautions
TCM dietary therapy for mononucleosis rests as much on what must be avoided as on what must be prescribed. Each phase has its own food prohibitions, non-compliance with which can prolong the illness or trigger relapses.
| Aliment | Nature | Saveur | Méridiens | Actions | Précautions |
|---|---|---|---|---|---|
| Acute Phase (Day 1-14) | To be absolutely avoided | Alcohol, fried foods, strong spices, refined sugar, dairy products | To be strongly limited | Red meats, cold raw vegetables, coffee | Alcohol and fried foods nourish Heat; dairy products generate Phlegm-Dampness |
| Convalescence Phase (Day 15-45) | To be absolutely avoided | Alcohol, excess sugar, processed foods | To be strongly limited | Excess warming spices, raw vegetables in large quantities | Refined sugar inhibits Spleen Qi reconstruction |
| Chronic Phase (Day 45+) | To be absolutely avoided | Excess cold raw foods, prolonged fasting, restrictive diets | To be strongly limited | Excess coffee, irregular meals, emotional snacking | Fasting and restrictive diets further deplete already weakened Qi |
Matrix of absolute contraindications and limits - Yin Shi protocol
Alert Signs Requiring Immediate Readjustment
- Fatigue worsening after a meal: reduce animal proteins, increase cooked cereals and vegetables. The Middle Jiao cannot transform heavy proteins.
- Persistent bloating, loose stools: check for excess Dampness-producing foods (dairy, sugar, fats). Temporarily switch to pearl barley (Yi Yi Ren) and white radish congee.
- Fever or sore throat reappearance: temporarily return to Phase 1 principles (clarification) for 48 to 72 hours before resuming tonification.
Integration with Other TCM Modalities
Chinese dietary therapy reaches its full potential when coordinated with other branches of TCM: herbal medicine, acupuncture, cupping, and energetic exercises. The therapist must schedule food intake relative to therapeutic sessions to optimise assimilation and avoid antagonisms.
| Aliment | Nature | Saveur | Méridiens | Actions | Précautions |
|---|---|---|---|---|---|
| Herbal Medicine | Support dietary strategy | Yin Qiao San (acute phase), Bu Zhong Yi Qi Tang (convalescence), Liu Wei Di Huang Wan (Yin Deficiency) | Adapt foods to formula properties | Avoid cold foods with warming formulas; avoid heating foods with clarifying formulas | Schedule meals 1 hour before or 2 hours after decoctions |
| Acupuncture | Circulate Qi/Blood, tonify the Root | E36 (Zu San Li), SP6 (San Yin Jiao), LI4 (He Gu), LU7 (Lie Que), Shu points of the back | Schedule meals 1 hour before or 2 hours after sessions | Optimise assimilation by avoiding heavy meals immediately after a tonifying session | Do not fast before a deep tonification session |
| Cupping / Gua Sha | Disperse Toxic Heat, unblock meridians | Bladder line, interscapular zone | Slightly increase warm liquid intake after sessions | Clear vegetable soup or warm chrysanthemum infusion within the hour following the session | Avoid cold or iced foods that would contract the freshly stimulated meridians |
| Qi Gong / Gentle Exercises | Reconstruct Qi without exhausting | Ba Duan Jin, abdominal breathing exercises | Eat lightly 1 hour before practice, nourishing meal within 45 minutes after | A warm congee post-practice promotes Qi return to the Middle Jiao | Avoid intense physical exertion that disperses convalescent Qi |
Dietary coordination with TCM modalities - Yin Shi protocol
Follow-up and Evaluation: Clinical Indicators
Dietary management of mononucleosis requires regular follow-up and objective evaluation of energy progression. The TCM therapist must document the following indicators at each consultation to adjust the dietary prescription.
Evolution Grid to Document
- Pulse Quality: does it progress from rapid and slippery (acute phase) to thin and weak (Qi deficiency) then to full and regular (reconstruction)?
- Tongue: does it return to a pink colour and thin white coating? A persistently red tongue without coating beyond 3 weeks signals unresolved Yin Deficiency.
- Digestion: do meals trigger bloating or loose stools? Regular formed stools are a reliable indicator of Spleen motive force returning.
- Daytime Energy: fewer post-meal crashes, ability to get through a day without mandatory afternoon rest.
- Physical Activity: progressive return to daily 30-minute walk without exhaustion the following day.
Conclusion: Holistic and Personalised Approach
Dietary management of mononucleosis in TCM rests on three fundamental pillars, applicable regardless of the patient’s individual pattern.
- Precise Differentiation: Do not treat mononucleosis as a fixed entity, but the individual energy pattern at a given time T. Dietary prescription fundamentally changes between the acute phase (dispersion) and the chronic phase (tonification).
- Evolutive Adaptation: Adjust recommendations to each clinical phase without rigid protocol. Weekly or bi-weekly consultation allows progression adjustment before a dietary error becomes a major obstacle.
- Therapeutic Education: Equip the patient so they become an actor in their convalescence. Simple dietary markers (tongue, stools, post-meal energy) allow them to self-manage their daily adaptation without depending solely on consultations.
Nourishing the body with discernment is better than treating illness with potions. Convalescence is the art of transforming food into medicine through choice, measure and timing.
FAQ: Answers for Featured Snippets and Voice Search
What TCM diet in acute mononucleosis phase?
In the acute phase (first 2 weeks), prioritise fresh and liquid foods that clear Toxic Heat: pear, watermelon, melon, cucumber, mung beans (Lu Dou), chrysanthemum. Absolutely avoid fried foods, alcohol, strong spices, dairy products and refined sugar that nourish Heat and generate Dampness.
Can we tonify Qi from the convalescence phase onwards?
Not brutally. Convalescence (weeks 3 to 6) requires progressive introduction of tonifying foods. Begin with millet and brown rice congee, then progressively add farm chicken in broth (1 part protein to 4 parts cereal). Observe digestive tolerance before each increase.
Which foods reconstruct Yin after chronic mononucleosis?
Foods nourishing Liver and Kidney Yin are prioritised: organic egg yolk, squid, blackberry, moderate goji berries, black sesame, spinach, beetroot. Avoid long cooking and warming spices that further consume Yin. Sweet, warm, slow-cooked preparations are optimal.
What symptoms indicate a dietary phase change?
Three clinical signs guide the transition: the tongue passing from red with thick yellow coating to pink with thin white coating (exit from acute phase); reappearance of loose stools after protein introduction (slow down tonification); persistence of night sweats despite treatment (Yin Deficiency, requires Yin-nourishing foods).
Can Chinese herbal medicine alone treat mononucleosis?
TCM herbal medicine is a powerful complement but does not replace medical monitoring. The formulas Yin Qiao San (acute), Bu Zhong Yi Qi Tang (convalescence) and Liu Wei Di Huang Wan (chronic) must be prescribed by a certified practitioner and coordinated with the treating physician. Dietary therapy supports their action and reduces digestive side effects.
How to differentiate Qi Deficiency fatigue from Yin Deficiency fatigue?
Qi Deficiency manifests as physical fatigue on exertion, spontaneous sweating, pale tongue and weak pulse. Yin Deficiency is accompanied by night restlessness, night sweats, dry mouth in the evening, red tongue without coating and thin rapid pulse. Dietary prescriptions are opposite: Qi requires warm, tonifying cereals; Yin requires moist, fresh foods.
Document written for professionals of Chinese energy dietary therapy. Synthesis based on TCM classics, modern protocols from the Academy of Nanjing, and contemporary integrative medicine data. Last updated: April 2026.